Parathyroid Surgery
For primary hyperparathyroidism, the only cure is an operation.
Fortunately, when performed by an experienced surgeon, the operation is a quick outpatient procedure - meaning that you can go home the same day, no need to stay overnight at the hospital.
During the operation, one or more diseased parathyroid glands are removed. Primary hyperparathyroidism is most often caused by a benign tumor on one or two of the parathyroid glands. Removing those glands, and leaving the other normal glands behind, cures the disease.
Sometimes, all four parathyroid glands are diseased, and we need to remove three parathyroid glands and part of the fourth during the operation. We never want to remove all four parathyroid glands, because you do need some parathyroid hormone to keep your calcium in normal range.
There are no medications that cure primary hyperparathyroidism. There are medications that can help bring your calcium levels down if they are extremely high, but this is a temporary measure and should be followed up with surgery when possible.
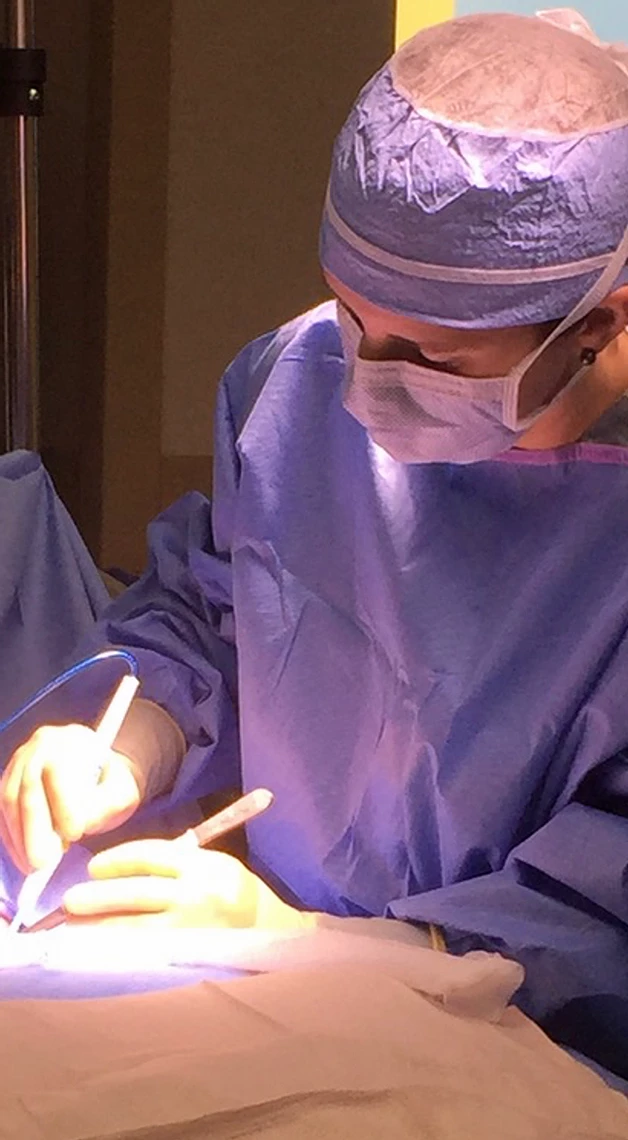
What We Do: Minimally Invasive Direct Visualization of All Parathyroids
Dr. Boone directly examines all four parathyroid glands in nearly every patient. This is done through a minimally invasive approach with a 1-inch skin incision at the base of the neck. Direct visualization, seeing all of the glands in the operating room, is the best way to ensure that the diseased glands are removed and the remaining glands are healthy. There is no substitute for actually visualizing all of the glands.
Unfortunately, this is not how most parathyroid operations are done. Most parathyroid operations today are "focused" or single-gland operations, in which the surgeon only looks at and removes the one parathyroid gland seen on a preoperative scan. Many patients just have one diseased parathyroid, but up to 30% have multiple diseased glands, and they will not be cured with a focused operation. Surgeons often prefer to do focused operations because they are not experienced in four-gland operations, and were never taught how to find and evaluate the parathyroid glands. This was true for Dr. Boone in training - she was only taught to do focused parathyroid operations. Now, after performing thousands of four-gland parathyroid operations, she only rarely recommends a focused operation. Most patients are better served by having all four parathyroids seen, if the surgeon has the experience to do this quickly and safely.
When having surgery at our center, you will speak with Dr. Boone in the preoperative area to go over the plan and discuss any concerns. She will give you the postoperative instructions and review these with you. The operation lasts about a half hour and is done as an outpatient procedure. After the operation, Dr. Boone will update your family, and once you are awake she will go over the findings with you as well. Most people can go home or back to the hotel within about 2 hours after the procedure. You cannot drive yourself home, so you will need a friend or family member to help. If you are coming from out of town, we prefer that you stay in the Phoenix area the night of surgery. You can fly or drive home the next day. Dr. Boone calls every patient the evening of surgery, to say hi and ask if you have any issues or questions. You will also be given her cell phone number and email address in case you have any questions later.
Approaches to Parathyroid Surgery
Surgeons have different ways of doing parathyroid operations. We will cover the most common approaches here, along with the benefits and risks of each, and when you might want to use them.
Open vs. "minimally invasive"?
When you read about parathyroid surgery, you may see it described in various ways, and the terminology can be confusing.
With regard to parathyroid surgery, the terms open and minimally invasive do not have a concrete definitions. It usually refers to incision size - if the incision is small, it is called minimally invasive, and if the incision is large, it is called open. Most parathyroid operations are "minimally invasive" because they can be done through small (1 to 2 inch) neck incisions, even if both sides of the neck are opened during a four-gland operation.Note about risks: All operations have risks. We operate when we believe that the benefits of surgery outweight the risks of the operation. The risks of parathyroid surgery generally are minimal, but are not zero. All of the surgical approaches listed below have the potential for complications. The risk of complications is not correlated with the surgical approach, but with the surgeon's level of experience. To give yourself the best chance of a good outcome, choose the surgeon with the most experience.
1. Direct Visualization of All Parathyroids
In this method, the surgeon opens the neck and examines all four parathyroid glands, two on each side. This is usually done through a minimally invasive (1 inch) incision. This method will fully expose the thyroid and surrounding structures in the neck. Since many patients (about 30%, and more in older patients) will have multiple parathyroid glands involved, this is a good method of viewing all of the glands together and determining which need to be removed. This can be done through a 1 to 1.5 inch neck incision in most people. When all four glands have been seen, or a thorough attempt has been made to see all four, and the abnormal glands have been removed, the operation is concluded.
-
Benefits of four-gland approach:
- This method has the highest cure rate in experienced hands. Small diseased parathyroid glands that were not seen on imaging will be found and removed.
- The parathyroid glands do not need to be seen on imaging studies. Often, parathyroid tumors cannot be seen on any scans. With a four-gland approach, it is not necessary to know which parathyroid gland or glands are the problem before the operation, since all four will be evaluated anyway.
- The surgeon can ensure that the only glands remaining in the neck are normal glands. Without actually seeing them, it is not possible to confirm that the glands are normal.
- The thyroid can be fully evaluated at the same time as the parathyroid operation. Thyroid nodules are common, and they are usually benign. Sometimes larger or suspicious nodules will need to be removed to fully evaluate them, and this can be done during parathyroidectomy.
- This method is essential for conditions that cause hyperplasia (MEN syndromes, secondary hyperparathyroidism, and tertiary hyperparathyroidism) or are associated with high rates of multigland disease (normocalcemic primary hyperparathyroidism, lithium-associated primary hyperparathyroidism, and familial hyperparathyroidism).
- For inexperienced surgeons, the operation is longer than a focused procedure, since there is more dissection and all four glands need to be found. Experienced surgeons should be able to find all four parathyroid glands in most people in under 30 minutes. Inexperienced surgeons are less likely to be able to find all four glands, even with extensive dissection.
- Particularly for inexperienced surgeons, there is an increased risk of complications, such as voice changes due to dissection around the recurrent laryngeal nerves (you have one on each side of the neck - these nerves control your vocal cords)
- Potentially increased risk of hypoparathyroidism, especially for inexperienced surgeons: this occurs when all of the parathyroid glands have either been removed or damaged. It is a condition of chronically low calcium that can significant reduce quality of life. If the surgeon is exposing all four parathyroid glands and is not careful with them, there is a risk that the glands will be damaged.
2. Focused parathyroidectomy
Since most people with primary hyperparathyroidism will have just one diseased parathyroid gland, some surgeons choose to operate only on one gland. The gland is identified before the operation with an imaging study, such as sestamibi, CT, or ultrasound. The surgeon focuses only on that gland and removes it. The operation is over once that gland is removed.
Benefits of focused parathyroidectomy:- Surgeons do not need to be experienced in finding parathyroid glands. Finding normal parathyroid glands can be quite challenging, and surgeons who do not do it often may have difficulty finding the glands. A focused operation is a good approach in this case.
- Since the surgeon is only operating on one spot, he or she will only be entering only one side of the neck, avoiding any possibility of damaging the other side.
- Lower cure rates: Many patients will have multiple diseased parathyroid glands. The overall percent is about 25 to 30%, but the risk rises with age. Over a third of patients older than age 80 will have more than one diseased parathyroid gland. These patients will not be cured with a focused operation. Often, the imaging studies will only show the largest parathyroid tumor - the second tumor may not be seen at all on scans.
- Potential need for second operation: If there is a second (or third) tumor that is not seen during the focused procedure, the patient will need another operation at a later time. Some individuals are at higher risk for complications of anesthesia, and may not want to undergo another procedure.
- Inability to evaluate the thyroid: the thyroid cannot be fully evaluated. There is a higher chance of missing a small thyroid cancer that would be identified during a four-gland operation.
3. Focused parathyroidectomy with intraoperative PTH (ioPTH)
In this method, the surgeon starts out with a focused operation. She uses imaging to guide her to which parathyroid gland needs to be removed. Just before removing the diseased gland and then after, she checks the blood PTH level. If the PTH level drops by a certain amount (usually 50%, and/or into the normal range), the operation is finished. If the PTH does not drop enough, she continues with a four-gland operation. PTH levels generally drop very quickly when a parathyroid tumor has been removed. Theoretically, if there is another tumor present, the PTH will not drop at all or as quickly. For this approach, the operation continues until the PTH drops or the surgeon has exhausted all attempts to get the PTH down.
Benefits of ioPTH-guided focused parathyroidectomy:- Surgeon feels reassured that he or she removed a parathyroid tumor before leaving the operating room.
- Longer time under anesthesia: PTH results can take anywhere from 10 minutes to 25 minutes to get a result. Typically the PTH is checked at 5 minutes after removing the parathyroid tumor, then at 10 minutes, then 15. If the PTH drops by minute 15, and the PTH takes 20 minutes for results, then the patient is under anesthesia for an additional 35 minutes - while essentially nothing is happening.
- PTH can drop by 50% even if there is another tumor present. This is not uncommon, especially when there is one large tumor and one small tumor. The large tumor is the one currently making most of the PTH, so removing it causes the PTH level to drop dramatically. Then once the big one is gone, the little tumor takes over. Many parathyroid reoperations are done in patients who had ioPTH-guided operations. The PTH dropped by 50% and the surgeon quit the operation. And then a few days later the calcium and PTH were high again, and the patient needed another operation. The PTH was not a reliable indication of cure.
- PTH can take longer than 15 minutes to drop appropriately. In textbooks the PTH has a half life of under 5 minutes, but in reality it can take a half hour or more to see the PTH drop to where you want it. Some patients are cured after removal of one tumor, but the PTH doesn't "act like the textbooks." The patient then gets a much more extensive operation than she needs, while the surgeon then explores both sides of the neck. This increases the length of the procedure and the risk of complications, particularly if the surgeon is not used to doing four-gland operations.
4. Radioguided parathyroidectomy
Also called Minimally Invasive Radioguided Parathyroidectomy, or MIRP. This is a variation on the above approaches. With this technique, the patient must have an injection of a radioactive tracer like technetium-99 just prior to the operation (usually as part of a sestamibi scan). The parathyroid glands take up the radioactive tracer and are thus temporarily radioactive. The amount of tracer that they take up depends on how active they are (and therefore how diseased they are), so a parathyroid tumor will have a higher radioactivity level than a normal gland.
One thing to note is that radioactivity cannot be measured while the gland is still in the neck, because there is too much background radioactivity from the thyroid (the thyroid also takes up the radioactive tracer). It can only be measured once the gland (or part of the gland) has been removed. The surgeon can take a biopsy of gland (cut off a tiny piece) and measure the radioactivity level. If the level is low, the gland is likely normal. If it is high, the gland is more active than it should be. This can help the surgeon determine whether the gland is diseased, particularly in cases in which the gland is not clearly normal or abnormal. The operation is concluded when all four glands have been evaluated.
- The radioactivity of each gland (or rather, a small biopsy taken from the gland) gives a real-time assessment of how "active" the gland is
- For surgeons who are not comfortable identifying parathyroid glands, the radioactivity level of a piece of the gland can help confirm that the tissue is parathyroid
- If there is a delay of more than a couple hours between the radioactive tracer injection and the operation, the radioactivity level is not as accurate, because it drops quickly over time. The radioactivity level in this case is unreliable.
- Radioactivity is not as helpful in cases of parathyroid hyperplasia. Hyperplastic parathyroids generally have a lower radioactivity level than adenomas, and the level can be within the range of normal glands. The surgeon may be falsely reassured by a radioactivity level that matches a normal gland.
- Though one can make generalizations about radioactivity levels in normal, hyperplastic, and adenomatous parathyroids, in reality there can be significant overlap between all of them, making the levels less helpful in many cases.
- Radiation: this procedure requires an injection of a radioactive substance. While it is a "low" dose, these doses add up over time to affect your health.
5. Scarless parathyroidectomy
This is called scarless because there is no neck scar. Incisions are made in other places and then the surgeon tunnels under the skin and muscle to get to the base of the neck. Given the amount of dissection, it is hard to call this minimally invasive. Despite not having a scar on your neck, there is a lot of internal scarring produced. There are a couple of ways to get to the parathyroids: surgeons can make an incision in either the axilla (armpit) or inside the lower lip. If going through the axilla, the surgeon may also make an incision around the nipple (periareolar) and a "robot" is often utilized (the robot is essentially a set of tiny arms controlled by the surgeon). If going through the inside of the bottom lip, it is called a "transoral" approach. Both approaches require the surgeon to tunnel under the skin and muscle, leading to scarring all through the tracts that are created.
Benefits of scarless parathyroidectomy:- There is no scar on the front of your neck.
- Potentially lower cure rate, since usually only one side of the neck is evaluated.
- Longer duration of operation: the setup and extra dissection generally leads to longer operations
- Increased internal scarring: all of the dissection under the skin and muscle causes internal scarring which can make future operations more difficult
- Few surgeons have experience with the technique. Very few perform it regularly, increasing the potential for complications.
- The complication rates are not fully known, given the relative infrequency of these procedures.
- The cosmetic benefit may not be significant: Most patients who have the more standard neck incision usually have a 1 inch horizontal line across the middle of the lower neck, which fades with time and is often hard to see after a year
Choosing the right approach
The optimal parathyroid procedure depends on the patient and the surgeon's experience. The operation routinely performed at our center is the Minimally Invasive Direct Visualization of All Parathyroids. This is typically done through a 1 to 1.5 inch incision, and all four parathyroid glands are evaluated. Most operations are less than half an hour. For first-time operations (when the patient has not had prior neck surgery) this is the method that will give the highest chance of cure. We have found numerous parathyroid tumors that would not have been found with a focused approach, because they were never seen on a scan.
There are situations when a focused operation is the best approach. Because finding all four parathyroid glands can be very challenging, surgeons who have minimal experience with this should perform focused operations. If finding the glands could take four hours, then the surgeon is better off just going after the one gland seen on scan.
There are select scenarios when we will perform focused operations at our center:
- Young patients. Teenagers and young adults in their 20s with spontaneous primary hyperparathyroidism typically have one adenoma. It is unusual for them to have two tumors. Thus, if a scan shows one tumor, we prefer to just look on one side of the neck. We can remove the tumor and confirm that the other gland on that side is normal - if it is not, then we need to look at all four glands. Doing a unilateral (one-sided) operation reduces the risk of complications and avoids creating scar tissue on the other side.
- Reoperative cases. When someone has already had a parathyroidectomy and needs another, it is often not possible to see all of the remaining glands, as they are stuck deep in scar tissue. Doing a lot of dissection to expose them risks injuring nearby structures like the recurrent laryngeal nerves, which control the vocal cords. For reoperative cases in which both sides of the neck have already been opened, we will usually plan to just go after the tumor seen on scan.
We do not use intraoperative PTH at our center. In theory, it provides some reassurance that the person is cured without having to see all four glands. Unfortunately, as discussed above, it is often inaccurate, and we believe its use can lead surgeons to make poor decisions (either digging around more than they should because the PTH took a while to drop, or stopping the operation when another tumor was present because the PTH dropped quickly). In most cases, it also significantly prolongs the operation and time under anesthesia, while surgeons wait for PTH results. For these reasons, we do not recommend the routine use of ioPTH.
Using radioguidance can be helpful in some situations. At the Norman Parathyroid Center, where Dr. Boone started, all operations were performed with radioguidance. When starting out, it was very nice to be able to measure the radioactivity of every parathyroid. As she gained experience, she realized that radioguidance was a crutch, similar to ioPTH, which made the surgeon feel better but added little to no value for the patient. For most patients, it didn't help at all. Once a surgeon is experienced enough to find the parathyroids and has looked at enough to accurately assess them, radioguidance is not necessary. While sestamibi scans are invaluable for planning parathyroid surgery, it is not necessary to perform a separate scan or injection of radioactive material on every patient on the day of surgery.
If you would like to pursue surgery with Dr. Boone, the first step is to schedule a consultation.
Not sure if you need surgery? If you need help figuring out your calcium and PTH results, try our free Parathyroid Disease Analysis Tool.